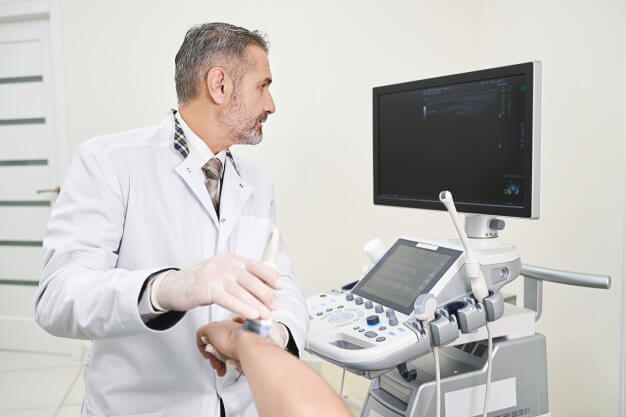
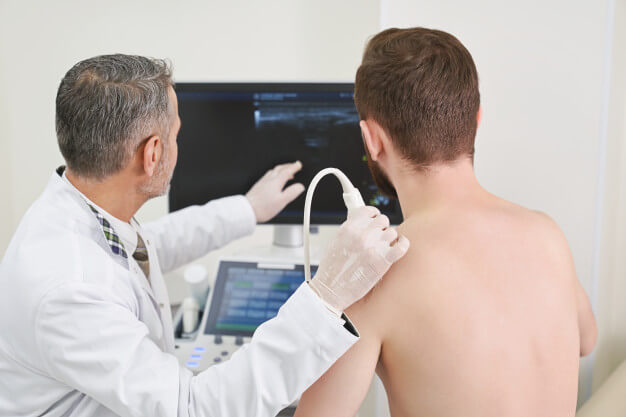
Running a hospital or a clinic requires you to be able to provide only the best tools for your patients or clients. Only with equipment and apparatus that are guaranteed to work well all the time can you give everybody the kind of care that they need. This, of course, also applies to the probing tools that your hospital employs. Probes may indeed look small and just by looking at them, you get the impression that they are easily replaceable when broken or stop functioning. Assuming that they are indeed easily replaceable, would consider replacing all of the probes frequently a money-efficient kind of way to operate a hospital? Sure, you need to provide the best equipment for the patients but even when the price of probing tools is affordable, you should never replace one regularly. What seems affordable at first may pile up and become something that you need to reconsider all over again. This also applies to the ultrasound transducer probe that the hospital you run operates. Now and again, the tool will receive tear and wear and you should always repair it whenever possible. Replacement is something you can consider when the tear and wear on the tools are so severe that the tool could put a patient’s life in danger when introduced to said tool.
Of all ultrasound probing tools, the transesophageal probe is arguably the most sensitive and fragile one. A patient might bite down on the probe upon its insertion down said patient’s throat. Even when the tool does not suffer from getting bitten by a patient, several extraneous factors may lead it to deteriorated. As it gets disinfected frequently after each use, the surface may strip off. Storage and improper handling may also affect how the probe performs in the long run. It then becomes utterly important for you to find the help that can deal with such a problem. When it comes to looking for a repair service for the ultrasound probes you have in your hospital or clinic, you need to find out if the service company provides a comprehensive service that covers everything. It needs to be flexible and versatile so you know that your probe is in the right hand. Replacement of parts of the probe should encompass everything from bending the neck to the insertion tube and from the head to the wiring. Repair should cover the transducer cable and strain relief as well as the wiring sheath. Do not forget to check if the service company also offers repair services for the bite marks, especially on the insertion tubes. Check with the company on the matter of relabeling and recoating of insertion tubes as this part is arguably the most important thing because it helps a lot with the patient’s convenience upon insertion.
Above all, consult your service company about whether or not they have the kind of flexibility when it comes to the brand of the probe. Different hospitals operate different probes and it is crucial to find out if the service company can deal with different brands of the tools as well.
Read Also :